In conflict-affected settings, saving lives is only the first step. Access to reconstructive surgery is essential to restore function, dignity, and social participation for survivors of severe injuries, blast wounds, and extensive burns. Modern warfare generates complex, long-term injuries as a result of explosions from air or drone strikes and shelling attacks. These patients overwhelm first-line healthcare systems, creating critical gaps in surgical resources and delaying essential interventions such as debridement, amputation, and tissue reconstruction.
Several examples illustrate the scale of reconstructive and rehabilitation needs in contemporary conflicts. Researchers from Duke University, Guy’s and St. Thomas’ NHS Foundation Trust in London, and Al Shifa Hospital in Gaza found that as of May 2025, approximately 116,000 injuries were sustained in Gaza, with up to 46,000 requiring reconstructive surgery. In Ukraine, estimates suggest that over 50,000 war survivors require specialized reconstructive surgery. Broader rehabilitation data indicate that about 300,000 people have been registered with physical disabilities due to war-related injuries, highlighting both the immediate surgical burden and the long-term need for prosthetics, rehabilitation, and support for survivors to regain function and reintegrate into society.
Despite these immense needs, access to reconstructive surgical care remains extremely limited in many conflict-affected countries. The management of such patients requires a complex and coordinated continuum of care, from early identification and initial treatment to surgical intervention, prosthetic provision, rehabilitation, long-term follow-up, and sustainable financing.
A wide range of actors—including humanitarian organizations, healthcare professionals, local structures, and donors—are engaged across this continuum. However, these efforts are often fragmented, limiting their overall impact and leaving critical gaps in patient care.
Integrating reconstructive care into post-conflict and emergency health strategies is therefore crucial. This includes training first responders, establishing referral networks to specialized centers, and strengthening local surgical capacity.
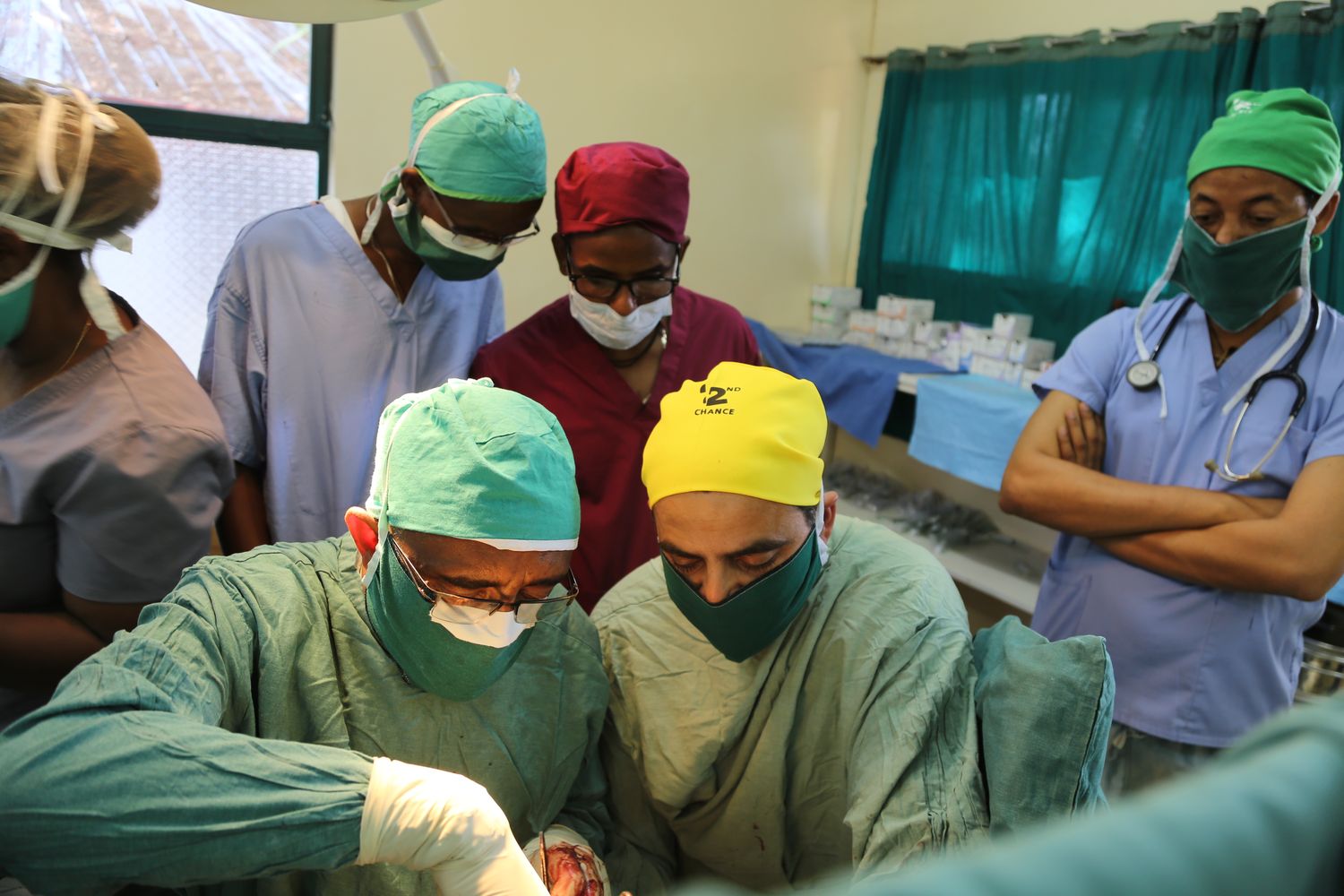

This workshop aims to:









| 14.00 | Opening remarks
|
| 14.15 | Field Perspectives. Presentations
Why and what have changed in modern conflict and new weapons ?
Integrated War Trauma Care in Ukraine: The Superhumans Model.
How to faciliatate access to surgery inside and outside Gaza ?
Field experience from Tigray and Sudan. |
| 14.45 | Breakout Group Discussions
|
| 15.30 | Coffee break and networking |
| 16.00 | Group Reporting & Next Steps |
| 16.45 | Closing Remarks
|
Registration is free but mandatory. The symposium will be held in person only (no virtual attendance).
She is a 30-year-old French photographer and videographer.
After working in the cultural sector for four years, she entered the humanitarian sector to give a voice to the most vulnerable people.
She had the opportunity to produce a documentary on the 40-year commitment of the NGO Première Urgence Internationale in Myanmar, where its work lies at the intersection of emergency aid and development.
In November 2025, she traveled to the DRC, specifically to Ituri and North Kivu, to document the NGO’s activities in the region, as well as the living conditions of thousands of families affected by the conflict.
Far from the sensationalist clichés people may have grown accustomed to, her work focuses on the resilience of communities, mutual aid, and the dedication of humanitarian workers.
Through this report, her goal is above all to remind audiences that behind the shocking statistics seen every day, there are individuals whose lives have been shattered by conflict.
To contact Tania RIeu : trieu@premiere-urgence.org
Cora Portais (b. 1993, Ivory Coast) is a Franco-Senegalese documentary photographer whose work engages with contemporary social, human, and political issues. Her practice explores the ways in which photography can bear witness to lived realities while questioning the power structures embedded in the production of images.
She began her photographic work at the age of 21 with a long-term project on access to education and healthcare for children with albinism in Senegal. The project received international recognition and was exhibited in Washington by the World Bank, as well as in Dar es Salaam and Nairobi, and presented during an international conference on albinism organized by the Open Society Foundation in South Africa.
Originally trained in journalism in France, where she worked with the Africa desk of Courrier International, Portais further developed her documentary approach in 2016 at The Market Photo Workshop in Johannesburg, a school founded by photographer David Goldblatt. There, she refined a socially engaged photographic practice while continuing her research on albinism and documenting marginalized urban communities in South Africa.
After returning to Senegal in 2017, she initiated several personal projects, including Etakaï, a series produced in Casamance that reflects on cultural transmission and the persistence of traditional practices within contemporary societies. In 2018, she was a semi-finalist in Magnum Photos’ Photography & Social Justice Program. Her work has since been presented in Europe and Africa, notably with the German gallery IkA, at the Iziko National Museum in Cape Town, and during festivals and the Off program of the Dakar Biennale.
Since 2019, Cora Portais has worked with the medical humanitarian organization ALIMA (The Alliance for International Medical Action), producing photographic documentation on public health issues in crisis contexts across the Sahel and Central Africa. Working in regions affected by conflict, displacement, and climate-related challenges – including the Central African Republic, Cameroon, and the Sahel – she documents themes such as epidemics, malnutrition, and maternal and child health.
Grounded in a sustained commitment to social justice, her work reflects on the ethics of documentary practice and the responsibility of the photographer in shaping visual narratives. Through long-term engagement and collaboration with the communities she photographs, Portais seeks to create images that move beyond representation to question how stories are told, who tells them, and for whom.
To contact Cora Portais : cora.portais@alima.ngo
The discussion at the World Health Assembly (WHA) is important because it aims to position health promotion as a central pillar of public policies, shifting from a care-centred approach to a comprehensive well-being approach based on action on the determinants of health and the engagement of all sectors of society.
A paradigm shift: from care to well-being
The document highlights a global framework for well-being (adopted in 2024) that seeks to reorient health systems towards health promotion, not only the treatment of disease. This implies recognising that health is primarily shaped by living conditions (social, environmental, and economic determinants).
A global policy priority under construction
The WHA discussion is key as it aims to firmly embed health promotion within policy agendas, in alignment with the Sustainable Development Goals and the Geneva Charter for Well-being.
Today, health promotion is still often secondary in public decision-making, despite being essential for building resilient and equitable societies.
A call for multisectoral and systemic action
The proposed framework emphasises an approach that “engages the whole of government and the whole of society.”
This directly strengthens approaches such as Health in All Policies and Healthy Cities, calling for transformation across governance, economic systems, and public policies.
An operational challenge: scaling up implementation
Finally, this discussion is strategic as it seeks to translate concepts into concrete implementation, through policy guidance, indicators, and actionable mechanisms for Member States.
👉 See preparatory document EB158/27 https://apps.who.int/gb/ebwha/pdf_files/EB158/B158_27-en.pdf
Five major approaches developed by the World Health Organization provide practical frameworks for acting on the determinants of health. They share a common objective: integrating health considerations across all public policies and living environments. By mobilising action at multiple levels — from local to global — these approaches aim to transform the conditions that shape health in everyday life. Together, they offer concrete levers to move from a care-oriented model towards a prevention- and equity-driven approach.
Social Determinants of Health framework
This foundational framework provides a comprehensive understanding of how social, economic, and political factors influence health outcomes and generate health inequalities. It distinguishes between structural determinants (such as governance, public policies, and social stratification) and intermediary determinants (including living conditions, behaviours, and access to services). It offers a conceptual basis for intersectoral action and is a key reference for addressing the root causes of health inequities.
👉 https://www.who.int/publications/i/item/9789241500852
Primary Health Care
Primary Health Care (PHC) is a whole-of-society approach to health that aims to ensure the highest possible level of health and well-being. It combines essential health services with action on the broader determinants of health, community empowerment, and multisectoral policies. PHC is central to achieving universal health coverage and reducing health inequalities by bringing services closer to where people live and by addressing their needs in a comprehensive way.
Creating Healthy Cities
This approach places health at the centre of local policies and urban governance. It encourages cities to act on key determinants such as urban planning, transport, housing, environment, and social cohesion. By engaging local authorities, stakeholders, and citizens, it promotes participatory and sustainable actions to improve health and well-being in urban settings.
👉 https://www.who.int/activities/creating-healthy-cities/creating-healthy-cities
Health in All Policies and intersectoral action capacities
This approach focuses on systematically integrating health considerations into all public policies (such as economy, education, transport, agriculture, etc.). The aim is to improve policy coherence and to act upstream on the determinants of health.
👉 https://www.who.int/activities/Promoting-health-in-all-policies-and-intersectoral-action-capacities
WHO urban health strategies
This global framework addresses the specific challenges of urban settings (inequalities, pollution, access to services). It is aligned with the Geneva Charter for Well-being, which calls for building well-being societies by acting on the structural determinants of health, and with the WHO global framework for integrating well-being into public health (2023–2024), which provides strategic guidance for transforming systems. These urban strategies promote integrated, evidence-informed action and collaborative governance to make cities healthier, more inclusive, and more resilient.
👉 https://www.who.int/publications/i/item/9789240116177
👉 https://www.who.int/publications/i/item/9789240084858
👉 https://www.who.int/publications/m/item/the-geneva-charter-for-well-being
15:30 – 17:30
This meeting is not open to the public.
It brings together stakeholders from Shanghai and Geneva who will explore opportunities for collaboration between Hospitals from Shanghai and Geneva University Hospitals.
12:30 – 14:30
This meeting is not open to the public.
It brings together stakeholders from Shanghai and Geneva who will explore opportunities for collaboration.
8:30 – 12:00
This meeting is not open to the public.
It brings together stakeholders from Shanghai and Geneva who will explore opportunities for collaboration.
The first session will explore the possibility of collaborating in the field of medical research.
The second session will explore opportunities for collaboration on tripartite projects involving China, Switzerland, and Africa. The role of digital tools in health programs and women’s health programs will be discussed in particular.
Established in 2006 by the University Hospitals of Geneva (HUG) and the University of Geneva (UNIGE), the Geneva Health Forum (GHF) is a Swiss not-for-profit initiative that brings together a diverse range of stakeholders to discuss and address global health challenges.
The GHF plays a pivotal role in the global health landscape, as a neutral and inclusive platform, fostering dialogue and collaboration among key players in the field, including policymakers, representatives from academia, civil society, and the private sector.
Its core mission is to facilitate constructive dialogue among these global health actors, which, in turn, contributes to the improvement of health policies and access to care worldwide. The Geneva Health Forum proudly collaborates with some of the most prominent international organizations based in Geneva.